A growing problem for health care institutions.
The subject of antibiotic resistance has garnered growing attention within health care institutions and organizations in recent years. Also known as multi-drug resistant organisms, antibiotic-resistance is an increasing problem for the health care sector.
In the 1980’s, it was thought that infectious diseases had been virtually banned through the use of antibiotics. Now, the World Health Organization has raised a red flag when it comes to antibiotic resistance. But what is antibiotic resistance and what causes it? Why is it a problem? And what does it mean for you in your work?
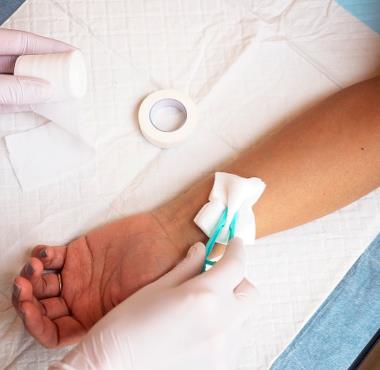
First aid for infection prevention
At Abena we help health care professionals prevent the spread of infections.
We do this by sharing our knowledge with health care professionals.
We help you to be alert to the transmission of pathogens, to take the right measures and to use the right products.
This way you minimize the risk of contamination.
What is antibiotic resistance?
Bacteria is everywhere around us. Everyone carries them with them, but you only get sick from some of these bacteria. Antibiotics are often dispensed to cure illness caused by bacteria. However, bacteria can become resistant to antibiotics, making it difficult to cure and care for infectious diseases. Antibiotic resistance has widespread consequences.
What is MDRO?
MDRO are multi-drug resistant organisms that are resistant to one ore more classes of antibiotics. The four most prevalent MDROs include: MRSA, ESBL, VRE, and CPE. Of these, MRSA is the best known.
Not everyone gets sick of a MDRO bacterium. You can also be a carrier. If you are a carrier you can infect others. Whether you become ill depends, among other things, on the immune system and the amount of microbes. The more microbes and the more aggressive the microbe, the greater the chance of becoming ill.
In addition, the immune system influences whether or not someone becomes ill. After an infection you may be able to get rid of the resistant MDRO bacteria. This depends on whether there is direct contact with the source and whether there are factors that increase the risk of carrier status (as is the case with MRSA for wounds and chronic skin diseases).
How do bacteria become resistant?
If antibiotics are used in an environment where only a few bacteria are resistant, only non-resistant bacteria are killed, or they cannot be multiplied by the antibiotics. The resistant bacteria remain and can multiply because they have less competition from, for example, nutrients.
Bacteria can also obtain resistance genes. Resistance genes can be transferred to antibiotic-sensitive bacteria in places where sensitive and resistant bacteria occur next to each other. For example, resistance genes from bacteria that usually do not cause infections in humans can be transferred to bacteria that cause infections.
Why do MDROs present a problem?
In January 2018, the WHO (World Health Organization) unveiled the first results of the research on antibiotic resistance. These results show high levels of resistance to a number of serious bacterial infections. This applies to both high and low income countries.
Some of the world's most common, and potentially most dangerous, infections caused by bacteria appear to be resistant to drugs. For example, 20% of people with a urinary tract infection have an infection whose bacteria are resistant to 7 of the 8 antibiotics. An inadvertently innocent infection can lead to many problems.
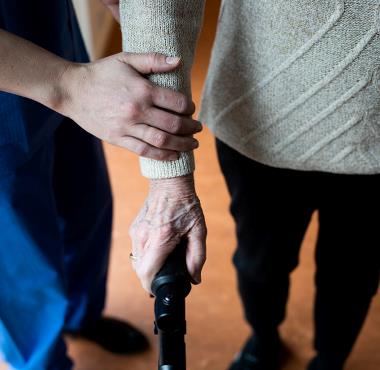
Hospital patients and nursing home residents: more at risk of MDRO
Because hospital patients and nursing home residents live relatively close to each other and often have a weakened immune systems, they are more at risk for contracting MDRO
In addition, they sometimes have poorer personal hygiene so that they run more risks of becoming ill. Age also plays a role: as the age gets older, the immune system functions less.
Consequences of MDRO for residents and patients
In general patients and nursing home residents with MDRO infections are sick for longer, require more care and have a higher risk of mortality.
In addition, patients feel discomfort and the feeling of being a burden or being ‘branded’ when they are MDRO positive. Once an infection is detected, MDRO procedures and protocols go into effect. Hospital patients or nursing home residents who are MDRO positive are cared for in isolation and with staff wearing specific protective clothing. Sometimes they also get a sticker on the door, so everyone is aware of the isolation case.
Consequences of MDRO for caregivers and family
MDROs also have consequences for hospital staff and caregivers. Care staff who are infected with a MDRO are generally not allowed to carry out surgical procedures or enter a department with patients or residents for a specific period of time. This can take between a number of months to sometimes years, although it varies per situation.
It not only has consequences for employment, but also for the family and the immediate environment of the caregiver. Family members and friends can also be infected, especially when taking care of a patient or loved one in a home care situation.
Use approved protective wear to protect the patient and the caregiver. Make sure you have the right products at your disposal – and you know how to use them. Read more about protective wear.
Gloves: Essential as protective device in healthcare, gloves come in various shapes and sizes. But not all gloves are suitable for working in healthcare. Which glove should you use, and how? Read more about gloves
Pay special attention to hand hygiene: Check out our guidelines for hand hygiene and find out why personal hygiene is essential in infection prevention.